Learning Health System Academy
The future of healthcare is digital.
Get ready with the Learning Health System Academy.
Meet the LHS Academy Fellows of 2023
University of Melbourne offers a new professional development program to equip clinicians with the skills to identify best digital health and data-driven practice and improve patient outcomes.
Designed by the Centre for Digital Transformation of Health, the Learning Health Systems (LHS) Academy teaches Fellows, through a mixture of coursework and practical project-based learning, to use health data to inform clinical practice and design, test, validate, implement and evaluate digital health-enabled models of care. Delivered in a hybrid format, Fellows participate in the program two days (Wednesdays, and one other day of choice) per week from early February to December.
Fellows gain skills and experience in using routinely collected clinical data to generate new knowledge and to design and implement digitally-enabled solutions to real clinical problems.
The Learning Health System Academy has been developed to:
- build our healthcare workforce capacity for data-driven and digital health-enabled clinical practice improvement
- truly transform healthcare through data-informed and technology-enhanced models of care
- enhance patient and end-user engagement in the transformation of health.

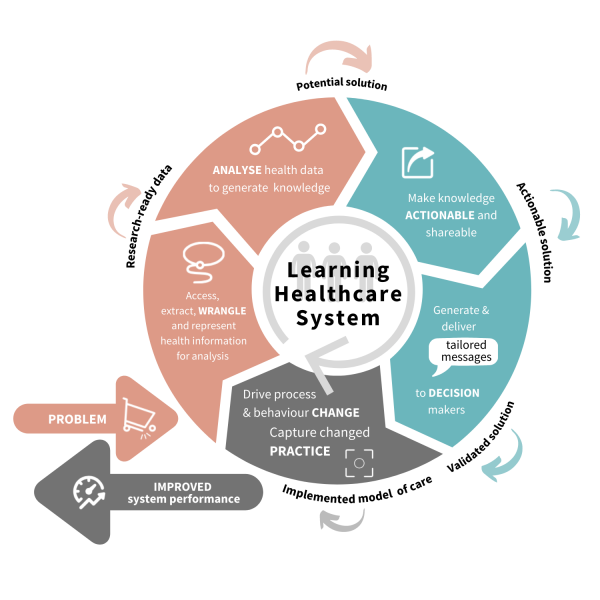
What is a Learning Health System?
Learning Health Systems are an accepted model for healthcare practice and quality improvement.
Learning Health Systems were originally defined by the Institute of Medicine as a system in which “science, informatics, incentives, and culture are aligned for continuous improvement and innovation, with best practices seamlessly embedded in the delivery process and new knowledge captured as an integral by-product of the delivery experience”.
Key features of a Learning Health System are:
- using data to generate new knowledge (D2K)
- using knowledge to inform clinical practice (K2P)
- evaluating changes in clinical practice (P2D)
Program Details
Information for Managers
Aim
The Learning Health System (LHS) Academy was developed by the Centre for Digital Transformation of Health (CDTH) at the University of Melbourne (UoM) to build capacity within health services to support moving towards an LHS approach to clinical practice, quality, and safety improvement. In particular, the LHS Academy is designed to start to build a critical mass of digital health and clinical informatics knowledge and skills to move towards a learning health system and nurture future leaders in digital health and clinical informatics. It’s not anticipated that the problem will necessarily be solved within the 12 months, more likely that a pilot phase of the project will be developed.
Position back-fill
The LHS Academy Fellow positions are partially funded by scholarships available from the CDTH. The health service will be required to arrange and fund back-fill for the reminder time release for 11 months. If the application is successful, details of the time-release and back-fill will be finalised between the applicant, unit manager, and CEO-nominated lead at the relevant health service.
Letter of support template
This letter of support template is to be downloaded, completed by the relevant unit manager, and submitted by the applicant together with the remaining required documents.
Health Service Leads - Clinical Informatics Director
CDTH Clinical Informatics Directors are located at each of MACH-affiliated site support on-site project-based learnings and implementation:
- A/Prof Jo-Anne Manski-Nankervis: Department of General Practice, University of Melbourne
- A/Prof Graeme Hart: Austin Health
- Dr Tim Fazio: Royal Melbourne Hospital
- Prof Karin Thursky: Peter MacCallum Cancer Centre
- Prof Jim Buttery: Royal Children’s Hospital
- Dr Oliver Daly: Western Health
Project
Applicants are required to identify a problem within their health service that could be addressed by a digital or data-driven solution. The internal shortlisting process by the CEO-nominated lead will ensure that this problem addresses an area of significant unmet need that aligns with service priorities, aligns with the digital health strategy, and that the applicant is an individual the health service wishes to foster as a future leader in clinical informatics and digital health.
Together with a CV and letter of support from the relevant unit manager this problem will form the basis of the application.
Application procedure
The selection process will be led by the Director for the Centre for Digital Transformation of Health, Professor Wendy Chapman. It will include shortlisting of applications by the CEO-nominated leads and interview by the health service and CDTH panel. The highly competitive program will welcome one successful application per MACH-affiliated health service, plus one GP, in 2024.
Pre-application inquiries may be sent to Meg Perrier, m.perrier@unimelb.edu.au.
Applications should be submitted by 5pm Monday 31st July 2023 via the application portal and must include:
- Completed LHS Application (via Qualtrics)
- CV (2 pages max), including brief details of any research projects undertaken, the applicant’s role in the research, and how findings were disseminated (report for supervisors, abstract presentation at meeting, publication etc).
- A letter of support from the Health Service divisional/operational/professional manager responsible to senior management for the clinician’s unit confirming;
- The applicant is well placed to develop an interest in clinical informatics and digital health,
- Has the potential to become a future leader of innovative care,
- Has in-principal support for two-days per week (Wednesdays, and one other day of choice) time-release from duties for 11 months if successful, and
- That the identified problem is important to address (please use letter of support template provided below).
The LHS Academy program has support from all MACH-affiliated health service CEOs. Each CEO has nominated a LHS Academy lead for their health service.
If the application is successful, details of the time-release will be finalised between the applicant, unit manager, and CEO-nominated LHS Academy lead at the relevant health service.
FAQs
-
Where do I submit my application?
Follow this link here
Submissions are via a Qualtrics form, with the option to add your CV and Letter of Support
Applications close 5pm Monday 31st July 2023. If you are unsure whether your application was successfully submitted, please contact Meg Perrier: m.perrier@unimelb.edu.au
-
What are the shortlisting selection criteria?
Shortlisting Selection Criteria
Each site will shortlist up to two applicants to move forward to interview, based on the following criteria:
- Is the applicant someone the health service wants to foster as a future leader in clinical informatics and digital health?
- Is the identified problem to be addressed an area of significant unmet need?
- Does the identified problem align with service priorities and the digital health strategy?
- Is the project a digital health project that lends itself to the learning health system framework?
Assessment Criteria for Panel (Health Service Lead/s and CDTH):
- Does the applicant have potential to become a future leader in clinical informatics and digital health?
- Is the identified problem suitably addressed by a digital or data-driven solution?
- Does the LHS model offer a feasible framework for solving the identified problem?
-
Is the LHS Academy assessed?
The LHS Academy is a non-credentialled professional development program. As part of the LHS Academy program, participants are enrolled in the Applied Learning Health System (ALHS) Short Course offered by the Centre for Digital Transformation of Health at the University of Melbourne. The remainder of the activity within the program is not assessed however attendance at workshops, micro-deliverables and final reporting will be required to fulfil conditions of the scholarship.
-
Does the release from duties need to be on a certain day of the week?
The program is designed to allow clinicians and EMR staff to be released from duties at a time that minimises disruption to service delivery. The LHS Academy requires participants to only be available on Wednesdays (fixed) and the remaining day is left flexible. The ALHS Short Course runs on Tuesday evenings between February and May via online delivery. For further details on the ALHS short course, please consult the website or contact the subject organiser, Dr Sathana Dushyanthen.
-
Meet the LHS Academy Fellows
The Learning Health Systems Academy is a structured and mentored year-long program designed by the Centre for Digital Transformation of Health and led by Professor Wendy Chapman to build career development pathways for aspiring agents of the digital transformation of health.
-
About the program
The LHS Academy equips Fellows with the knowledge and practical experience to design, implement and evaluate innovative digital change and lead data-driven continuous improvement in learning health systems. The program fosters interprofessional and research collaboration and provides experience in learning and working across boundaries to address common problems in digital health, using rigorous metrics and measuring outcomes to improve patient care and health service efficiency.
Through the 11-month program, clinicians are released from clinical duties for .4EFT (2 days per week) to upskill in digital health and clinical informatics through coursework, project-based learning and mentorship, while leading their project at their health institution.